How Does Workmen’s Compensation Work?
The purpose of Workmen’s Compensation is to provide compensation for disablement caused by occupational injuries or diseases sustained or contracted by employees in the course of their employment, or for death resulting from such injuries or diseases; and to provide for matters related to Injuries on Duty.
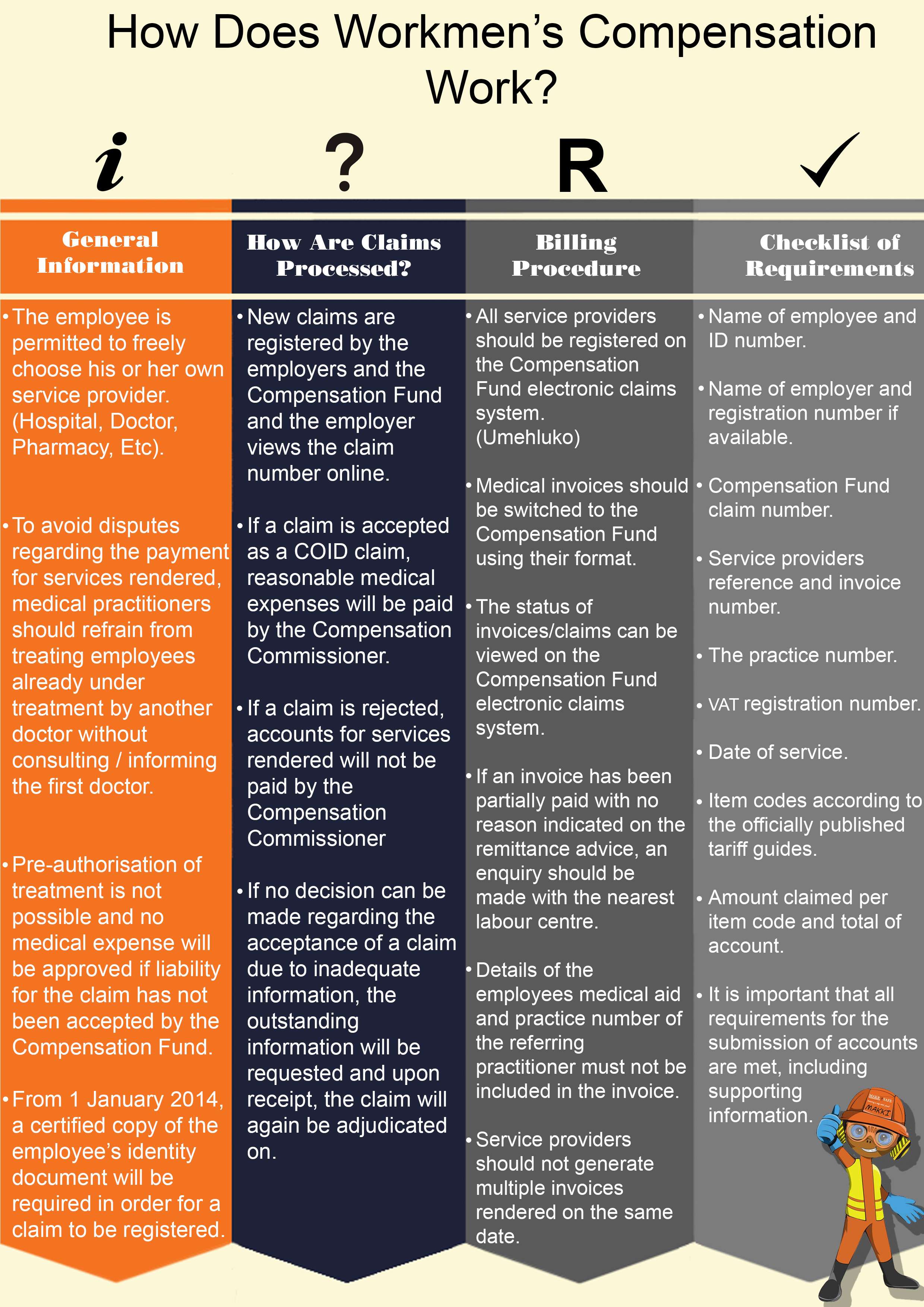
Here is everything you need to know about Workmen’s Compensation.
General Information
- The employee is permitted to freely choose his own service provider e.g. doctor, pharmacy, physiotherapist, hospital, etc. and no interference with this privilege is permitted, as long as it is exercised reasonably and without prejudice to the employee or to the Compensation Fund.
- To avoid disputes regarding the payment for services rendered, medical practitioners should refrain from treating an employee already under treatment by another doctor without consulting / informing the first doctor. As a general rule, changes of doctor are not favoured by the Compensation Fund, unless sufficient reasons exist.
- Pre -authorisation of treatment is not possible and no medical expense will be approved if liability for the claim has not been accepted by the Compensation Fund.
- From 1 January 2004 a certified copy of an employee's identity document will be required in order for a claim to be registered with the Compensation Fund. If a copy of the identity document is not submitted the claim will not be registered but will be returned to the employer for attachment of a certified copy of the employee's identity document.
How are claims processed?
- New claims are registered by the employers and the Compensation Fund and the employer views the claim number allocated online.
- If a claim is accepted as a COIDA claim, reasonable medical expenses will be paid by the Compensation Commissioner.
- If a claim is rejected (repudiated), accounts for services rendered will not be paid by the Compensation Commissioner. The employer and the employee will be informed of this decision and the injured employee will be liable for payment.
- If no decision can be made regarding acceptance of a claim due to inadequate information, the outstanding information will be requested and upon receipt, the claim will again be adjudicated on. Depending on the outcome, the accounts from the service provider will be dealt with as set out in point 2 and 3. Please note that there are claims on which a decision might never be taken due to lack of forthcoming information.
Billing Procedure
- All service providers should be registered on the Compensation Fund electronic claims system (Umehluko) in order to capture medical reports.
- Medical invoices should be switched to the Compensation Fund using the attached format.
- The status of invoices /claims can be viewed on the Compensation Fund electronic claims system. If invoices are still outstanding after 60 days following submission, the service provider should complete an enquiry form, W.CI 20, and submit it ONCE to the Provincial office /Labour Centre.
- If an invoice has been partially paid with no reason indicated on the remittance advice, an enquiry should be made with the nearest labour centre. The service provider should complete an enquiry form, W.CI 20, and submit it ONCE to the Provincial office /Labour Centre.
- Details of the employee's medical aid and the practice number of the referring practitioner must not be included in the invoice.
- Service providers should not generate multiple invoices for services rendered on the same date i.e. one invoice for medication and a second invoices for other services.
Checklist Of Minimum Requirements
- Name of employee and ID number
- Name of employer and registration number if available
- Compensation Fund claim number
- Service provider’s reference number and invoice number
- The practice number
- VAT registration number
- Date of service
- Item codes according to the officially published tariff guidelines
- Amount claimed per item code and the total of the account
Posted date: 29th Jan 2018
Latest News - Injuries on Duty (IODs) - Workmans Compensation 



Comments (7)
Hello I fell and hurt my hand at work, I want to see a doctor and possibly get an x-ray if suggested by the doctor. How do I find a list of doctors and/or medical facilities that will claim directly from the Fund so that I do not have to pay and them claim back myself? Thanks for any advice.
2024-11-04 11:42:54Hi Charlotte I'm sorry to hear about your injury. To find a list of doctors and medical facilities that can claim directly from the Compensation Fund, you can follow these steps: Contact Your Employer's HR or Safety Officer: They should have a list of approved medical practitioners and facilities that are registered with the Compensation Fund. They can provide you with the necessary information and guidance on the process. Visit the Compensation Fund Website: The Compensation Fund often has resources available online, including lists of accredited medical practitioners and facilities. You can check their official website for more information. Consult the Department of Labour: The Department of Labour in South Africa oversees the Compensation Fund. You can contact them directly or visit their website for guidance on medical facilities that accept direct claims. Ask for Recommendations: If you have colleagues or friends who have had similar experiences, they may be able to recommend doctors or facilities that handle direct claims from the Compensation Fund. Check with Medical Aid Providers: If you are a member of a medical aid, they may also have a list of practitioners who can assist with direct claims. Use Online Directories: Websites that list healthcare providers may also indicate whether they accept direct claims from the Compensation Fund. Make sure to inform the medical facility that you are seeking treatment for a work-related injury, as this will help them process your claim correctly.
2024-11-05 07:47:22Can a injured employee claim from the workman's comp
2023-05-27 00:10:01Good Day Samuel Thank you for reaching out and your query via our comments... You can claim if your IOD was registered with WCA and you have received a claim number, discuss the matter with your employer who needs to submit the claim as per WCA procedures... Follow this link for a FREE COIDA Service Book download: https://www.mysafetyshop.co.za/Products/COIDA-Service-Book-Version-23
2023-05-29 08:50:36what e-mail can be used to get hospital pre-auth for a procedure?
2025-02-19 15:26:29To whom it may concern. Regarding feed back on injury on duty how long is the waiting period & how does it work with regards to the payment for the injured (worker). Regards D.C Davies Have a lovely day ahead.
2023-02-23 06:06:12Dear Davina Thank you for your request via our comments... There is no specified waiting period with regards to payment for IOD. It is managed case by case and has many criteria that may effect the waiting period... It is always best practice to ensure all your paperwork and medicals reports etc are properly completed and submitted timeously to ensue a speedy pay out process... Please follow this link to read about our Injury on Duty and COID Support Package: https://www.makrosafe.co.za/The-Injury-on-Duty-and-Coid-Support-Package
2023-02-23 08:04:50Hi. My son fell down stairs at work and injured his left arm and left knee. His been off sick for a few weeks. He is now on light duty, but has recently complained of pain in his left upper stomach area, which is on the same side that he fell. The WCA doctors recon the pain is not related to the IOD, he suffered 2 months ago and refuse to treat him for that problem. His employer agree with the WCA doctors. Can this be true what the WCA doctors say and what can he do?
2024-01-21 08:50:29Dear John Thank you for your message via our comments... Sorry to hear about your sons IOD - Firstly, if your son has been off sick for 14 days or longer, then this IOD is regarded as a Sec 24 and must therefore also be reported to Department of Employment and Labour... If the doctors report is saying that the pain in the stomach is not related to the IOD, then my suggestion is to get a second opinion from another doctor... You might also want to contact WCA directly and lodge a "dispute", below are the contact details: Compensation Fund Operating Hours: 07:30 to 16:00, Monday to Friday. Telephone Number(s): 0860 105 350 Fax 0866889836 Call Centre: 0800 321 322 Street Address: Compensation House 167 Thabo Sehume Street, Delta Heights Building Pretoria Postal Address: P.O Box 955, Pretoria, 0001 Email Address CF-Complaints@labour.gov.za orcfcallcentre@labour.gov.za orcfenquiries@labour.gov.za
2024-01-22 09:30:13Please help with my father's compensation fund as he died and his file was with Lorraine at Pretoria My contact details is 0631844620
2019-11-17 04:43:30it would be convinient if the claims could be filled online like any othr claims to avoid lots of paper work. Currently any body has access to online info and with smart phones you can reach far and wide in terms of saving time and envirinment.
2022-04-08 11:36:55Dear Diketso Thank you for your reply and comment... Kindly follow this link to read about our Injury on Duty and COID Support Package: https://www.makrosafe.co.za/The-Injury-on-Duty-and-Coid-Support-Package
2023-02-23 08:06:24